
This is my sweet girl, Lila. She’s active and intelligent. She loves to swing, eat blackberries, and paint. Don’t you dare turn your back on her because she’s mischievous too! She loves her friends, family, and kitty-cats. She is absolutely the most wonderful thing I’ve ever done with my life, and she just so happens to have Down Syndrome.

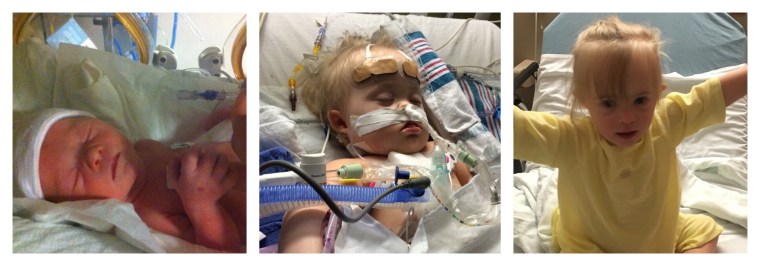
She might smile a lot, but her life hasn’t been easy. Born almost a month early due to multiple complications, Lila spent some time in the NICU. She’s overcome multiple illnesses and surgeries, including open heart surgery soon after her first birthday and many others since. In fact, we have received 2 new diagnoses this year alone, and she’ll have at least one surgery.
My husband and I are proud Arkansans. We’re educated, hard-working, tax-paying citizens. At the time of Lila’s birth, we lived in another state. Despite the fact that we both had good jobs and primary insurance coverage, we struggled to provide for her needs. When we moved back to Arkansas, Lila was significantly delayed in many areas.
 Our friends told us about TEFRA, a type of Medicaid funding that provides for disabled children and that requires the family to pay a premium. Our primary insurance pays first for all that it will cover, and Medicaid makes sure that Lila doesn’t go without the rest. We gladly pay a monthly fee for this essential assistance!
Our friends told us about TEFRA, a type of Medicaid funding that provides for disabled children and that requires the family to pay a premium. Our primary insurance pays first for all that it will cover, and Medicaid makes sure that Lila doesn’t go without the rest. We gladly pay a monthly fee for this essential assistance!
Lila now receives medical treatments that she needs from specialists and Occupational, Physical, and Speech therapy. She attends a school where she is loved and accepted, and they practice important skills in the classroom to prepare her for mainstream Kindergarten. Lila is constantly learning the necessary skills to be independent: speaking new words, learning to feed herself, to dress herself, and to climb stairs. One of my favorite moments was the first time I ever heard her say, “Ma Ma.” Can you imagine waiting 4 years to hear that?
 We never expected to need Medicaid. Even though we’d paid taxes for years for Medicaid, we didn’t know that a person’s life can change drastically in a moment – a car accident, a stroke, a job loss, a cancer diagnosis, a chromosomal difference – to cause them to need Medicaid. We thought that if we worked hard enough, we could take care of ourselves and Lila. But no matter how hard we work or what we give up, we just can’t afford to provide for all of Lila’s needs. Now, because of Medicaid, Lila is thriving, and we’re not being crushed under the weight of Lila’s ever-growing medical debt. We have hope that she will continue to develop and someday be a valued, contributing member of society. We are incredibly thankful for Medicaid.
We never expected to need Medicaid. Even though we’d paid taxes for years for Medicaid, we didn’t know that a person’s life can change drastically in a moment – a car accident, a stroke, a job loss, a cancer diagnosis, a chromosomal difference – to cause them to need Medicaid. We thought that if we worked hard enough, we could take care of ourselves and Lila. But no matter how hard we work or what we give up, we just can’t afford to provide for all of Lila’s needs. Now, because of Medicaid, Lila is thriving, and we’re not being crushed under the weight of Lila’s ever-growing medical debt. We have hope that she will continue to develop and someday be a valued, contributing member of society. We are incredibly thankful for Medicaid.
We tell everyone we can how essential Medicaid is! Lila has visited the Capitol and state lawmakers multiple times to represent herself and friends like her. Since she can’t speak much yet, my husband and I tell them how much Medicaid is literally saving lives. I can’t wait for the day that Lila will tell them herself. She brings a beauty and light to this dark world, and we will never stop fighting for her!


 My sweet boy, Ari, has had 2 shunt revisions, ETV placement and will be having a major skull reconstruction surgery in 2 months. He is still working on head control as well as feeding. He has overcome so much and he has so much further to go … without Medicaid he would not survive. Being a single parent, the support given through Medicaid help ensure that he will receive all the healthcare support that he so desperately needs. I work full time and have private insurance personally, he is also on my plan, but TEFRA helps allow for him to have continued therapy, the wheelchair that helps him participate in all community/school activities and surgeries that he needs to survive and thrive. His birthday is this week and I can’t believe he will be 4!!
My sweet boy, Ari, has had 2 shunt revisions, ETV placement and will be having a major skull reconstruction surgery in 2 months. He is still working on head control as well as feeding. He has overcome so much and he has so much further to go … without Medicaid he would not survive. Being a single parent, the support given through Medicaid help ensure that he will receive all the healthcare support that he so desperately needs. I work full time and have private insurance personally, he is also on my plan, but TEFRA helps allow for him to have continued therapy, the wheelchair that helps him participate in all community/school activities and surgeries that he needs to survive and thrive. His birthday is this week and I can’t believe he will be 4!!